Dangers of Pulling an Abscessed Tooth: What You Must Know in 2026
When it comes to oral health, an abscessed tooth is one of the most serious emergencies…
When it comes to oral health, an abscessed tooth is one of the most serious emergencies you can face. This painful condition occurs when a bacterial infection creates a pocket of pus at the root of your tooth or in the surrounding gum tissue. While tooth extraction might seem like the quickest solution, understanding the potential dangers and complications is crucial before making any decisions about your treatment.
The dangers of pulling an abscessed tooth include potential spread of infection, damage to surrounding teeth and bone, dry socket, nerve damage, and in rare cases, life-threatening complications. It’s essential to work closely with a dental professional who can properly drain the infection, prescribe antibiotics, and determine whether extraction is truly necessary or if the tooth can be saved through other treatments.
Understanding the Serious Dangers of Extracting an Abscessed Tooth
An abscessed tooth represents a severe infection that has penetrated deep into the tooth’s pulp chamber or spread to the surrounding bone and tissue. While extraction may sometimes be unavoidable, rushing into the procedure without proper preparation can lead to serious complications. Here are the primary dangers you need to understand:
1. Spread of Infection (Sepsis Risk)
The most dangerous complication of extracting an abscessed tooth is the potential spread of infection throughout your body. When a tooth is pulled while actively infected, bacteria can enter your bloodstream, potentially leading to sepsis—a life-threatening condition that requires immediate medical attention. This is why dentists typically prescribe antibiotics before attempting extraction of an infected tooth.
2. Damage to Adjacent Teeth and Structures
During the extraction process, especially if the tooth is severely decayed or the infection has weakened surrounding bone, there’s a risk of damaging neighboring teeth, their roots, or the jawbone itself. This can create additional problems that require further treatment and expense.
Why it helps: Using an antibacterial mouth rinse before and after dental procedures can help reduce bacterial load and support healing.
3. Dry Socket (Alveolar Osteitis)
Dry socket is one of the most painful complications following tooth extraction. It occurs when the protective blood clot that forms in the socket becomes dislodged or fails to form properly. With an abscessed tooth, the risk of dry socket increases because the infection can interfere with normal healing processes. If you experience severe pain days after extraction, you may be dealing with this condition.
4. Bone Loss and Structural Damage
When an infection has spread to the jawbone (a condition called osteomyelitis), extracting the tooth without properly treating the bone infection can lead to significant bone loss. This deterioration can affect your facial structure, make future dental work more difficult, and compromise the stability of neighboring teeth.
5. Nerve Damage
In rare cases, particularly with lower teeth, the extraction process can damage the inferior alveolar nerve that runs through your jawbone. This can result in temporary or permanent numbness, tingling, or altered sensation in your lower lip, chin, or tongue. While uncommon, this complication is more likely when extraction is performed on severely infected teeth with compromised surrounding structures.
What Actually Happens to an Abscess After Tooth Extraction
Understanding the healing process after extracting an abscessed tooth can help you know what to expect and identify potential problems early. Here’s what typically occurs:
Immediate Response (First 24-48 Hours)
Once the infected tooth is removed, your body immediately begins the healing process. A blood clot forms in the empty socket—this clot is absolutely critical for proper healing. During this time, you may experience swelling, mild to moderate pain, and some oozing of blood mixed with saliva. This is normal and expected.
The removal of the tooth also removes the primary source of infection, allowing your immune system to focus on clearing out remaining bacteria. If antibiotics were prescribed before the extraction, they continue working to eliminate the infection from surrounding tissues.
Early Healing Phase (Days 3-7)
During this period, white blood cells flood the area to fight any remaining infection and clean up debris. You might notice the extraction site appears whitish or yellowish—this is typically granulation tissue, not infection. The socket begins to fill in from the bottom up with new tissue.
If you’re experiencing persistent pain after 7 days, it’s important to contact your dentist as this could indicate a complication such as dry socket or residual infection.
Why it helps: Applying cold therapy to your jaw can significantly reduce swelling and discomfort during the first few days after extraction.
Intermediate Healing (Weeks 2-3)
By this stage, the socket should be mostly filled with granulation tissue, which appears pink and slightly raised. The tissue gradually matures and becomes firmer. Swelling should have subsided significantly, and pain should be minimal or absent. Your body continues to rebuild bone and gum tissue in the area.
Long-Term Healing (Months 1-6)
Complete healing of the bone and soft tissue can take several months. The socket gradually fills in with new bone, and the gum tissue reshapes itself. By six months post-extraction, the area should be fully healed, though you may notice a slight indentation where the tooth once was.
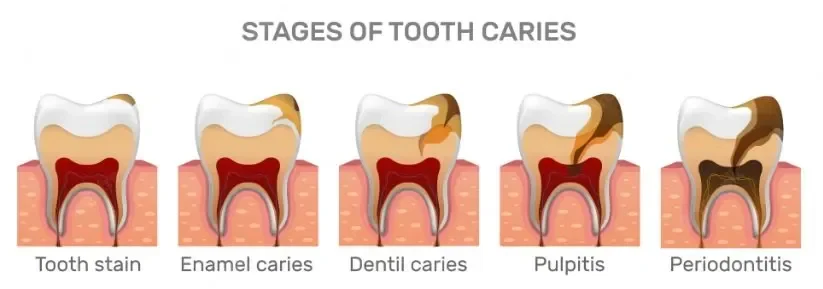
Recognizing the Stages of a Tooth Abscess
Understanding how a tooth abscess develops can help you seek treatment before it reaches a dangerous stage. Here are the progressive stages:
Stage 1: Initial Infection
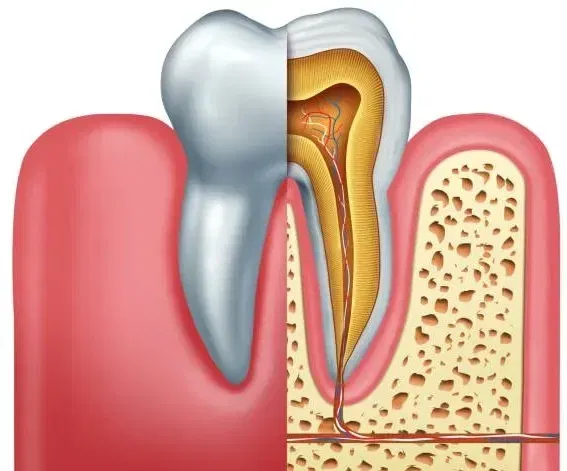
Bacteria enter the tooth through a cavity, crack, or chip, reaching the pulp chamber where nerves and blood vessels reside. You might experience increased sensitivity to hot and cold, mild pain, or discomfort when chewing. At this stage, a root canal can often save the tooth.
Stage 2: Abscess Formation
As bacteria multiply, pus begins to accumulate, creating pressure inside the tooth. Pain becomes more intense and constant. You may notice swelling in your gums near the affected tooth. The infection starts spreading through the root canals toward the tip of the root.
Stage 3: Advanced Infection
The abscess breaks through the bone and forms a visible swelling on your gums (sometimes called a gum boil or parulis). You might experience fever, difficulty opening your mouth, swollen lymph nodes in your neck, and a foul taste in your mouth. The tooth may appear darker than surrounding teeth. This stage requires immediate dental attention.
Stage 4: Complicated Infection
If left untreated, the infection can spread to your jaw, neck, or even other parts of your body. This is a medical emergency that can lead to cellulitis, Ludwig’s angina (a serious infection of the floor of the mouth), or sepsis. You may experience difficulty breathing or swallowing, severe facial swelling, high fever, and confusion.
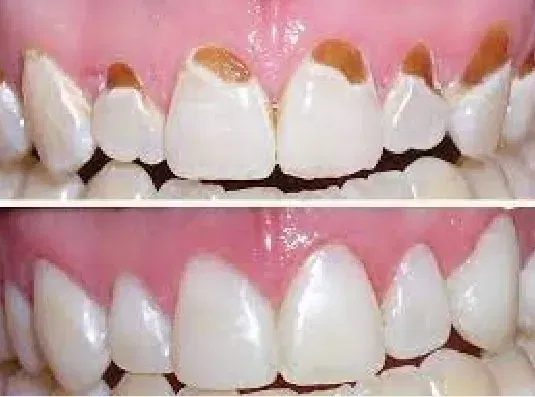
If you notice decay developing at your gum line, it’s crucial to address it promptly before it progresses to an abscess.
Why Antibiotics Are Essential Before and After Extraction
One of the most dangerous mistakes is attempting to extract an abscessed tooth without proper antibiotic coverage. Here’s why antibiotics are non-negotiable in these situations:
Pre-Extraction Antibiotic Therapy
Before extracting an infected tooth, dentists typically prescribe antibiotics for several days to reduce the bacterial load and control the active infection. This “pre-treatment” serves several critical purposes:
- Reduces infection spread risk: By decreasing the number of bacteria present, antibiotics minimize the chance of bacteria entering your bloodstream during extraction
- Decreases inflammation: Less inflammation makes the extraction procedure easier and less traumatic
- Improves anesthetic effectiveness: Infected tissue is more acidic, which can reduce the effectiveness of local anesthetics. Antibiotics help restore normal pH levels
- Protects overall health: For patients with certain medical conditions (heart problems, diabetes, compromised immune systems), pre-treatment antibiotics are especially important
Post-Extraction Antibiotic Coverage
After the tooth is removed, continuing antibiotics ensures that any remaining bacteria are eliminated. This prevents the infection from recurring and supports proper healing. Typically, you’ll need to complete the full course of antibiotics even if you start feeling better.
Dangers of Skipping Antibiotics
Extracting an abscessed tooth without antibiotic coverage significantly increases your risk of:
- Bacteremia (bacteria in the bloodstream)
- Sepsis and septic shock
- Spread of infection to facial spaces
- Osteomyelitis (bone infection)
- Delayed or incomplete healing
- Abscess recurrence in the extraction site
If you’re dealing with extreme tooth pain that’s keeping you awake, it’s crucial to see a dentist immediately rather than attempting any home remedies or self-treatment.
Why it helps: Following extraction, eating the right soft foods is crucial for healing while maintaining proper nutrition during recovery.
When Extraction Is Necessary vs. When the Tooth Can Be Saved
Not every abscessed tooth requires extraction. Modern dentistry offers several treatment options, and extraction should typically be considered a last resort. Here’s how dentists determine the best course of action:
Situations Where the Tooth Can Often Be Saved
- The tooth structure is largely intact with sufficient healthy tooth remaining
- The infection is confined to the pulp chamber and hasn’t severely damaged surrounding bone
- The tooth is strategically important for chewing or maintaining proper bite alignment
- You’re willing to invest in root canal therapy and a crown
- There’s adequate bone support around the tooth roots
Situations Where Extraction May Be the Best Option
- The tooth is severely fractured below the gum line
- Extensive decay has destroyed most of the tooth structure
- Severe periodontal disease has caused significant bone loss
- A vertical root fracture is present
- The cost of saving the tooth exceeds the cost of extraction and replacement
- You have a compromised immune system and the infection poses serious health risks
Proper Care After Extracting an Abscessed Tooth
If extraction is necessary, following proper aftercare instructions dramatically reduces your risk of complications:
First 24 Hours
- Bite on gauze for 30-45 minutes to allow clot formation
- Apply ice packs to reduce swelling (20 minutes on, 20 minutes off)
- Avoid rinsing, spitting, or using straws (suction can dislodge the clot)
- Take prescribed antibiotics and pain medication as directed
- Rest with your head elevated
- Stick to soft, cool foods
Days 2-7
- Gently rinse with warm salt water (after 24 hours) several times daily
- Continue antibiotics until the full course is completed
- Gradually introduce more solid foods as comfort allows
- Avoid smoking, alcohol, and strenuous exercise
- Keep the area clean but avoid brushing directly on the extraction site
Warning Signs That Require Immediate Attention
Contact your dentist immediately if you experience:
- Severe pain that worsens after day 3
- Fever above 101°F (38.3°C)
- Excessive bleeding that doesn’t stop with pressure
- Increasing swelling after day 3
- Difficulty breathing or swallowing
- Foul odor or taste that doesn’t improve
- Numbness that persists beyond the anesthetic wearing off
Conclusion: Making Informed Decisions About Your Dental Health
While the dangers of pulling an abscessed tooth are real and serious, working with a qualified dental professional who follows proper protocols can minimize these risks significantly. The key is never to delay treatment when you suspect an abscess, always complete prescribed antibiotic courses, and follow post-extraction care instructions meticulously.
Remember that tooth extraction should be considered carefully and is often not the only option. Modern root canal therapy has a high success rate and allows you to keep your natural tooth. However, when extraction is necessary, understanding the process, potential complications, and proper aftercare will help ensure the best possible outcome.
If you’re currently dealing with tooth pain or suspect you have an abscess, don’t wait—seek professional dental care immediately. Early intervention can often save your tooth and prevent the serious complications associated with advanced dental infections.